Are Your Digestive Symptoms Actually Ulcerative Colitis? Find Out in North Baltimore, MD
If you’re experiencing digestive symptoms and suspect ulcerative colitis, Dr. Nasseri MD, and his team at Nasseri Clinic offer professional evaluation and diagnosis. With advanced testing and personalized care, we help identify the cause of your symptoms and create an effective treatment plan to manage your condition and improve your quality of life. For more information, contact us or book an appointment online. We are conveniently located at 3333 N. Calvert St, Suite 540B, Baltimore, MD 21218.
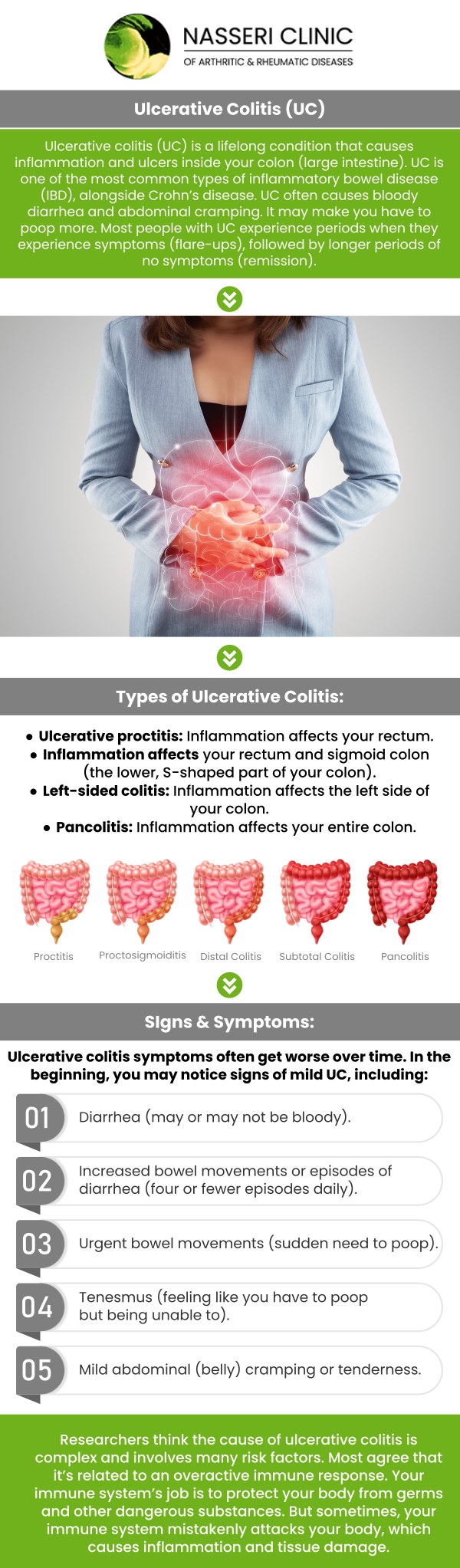
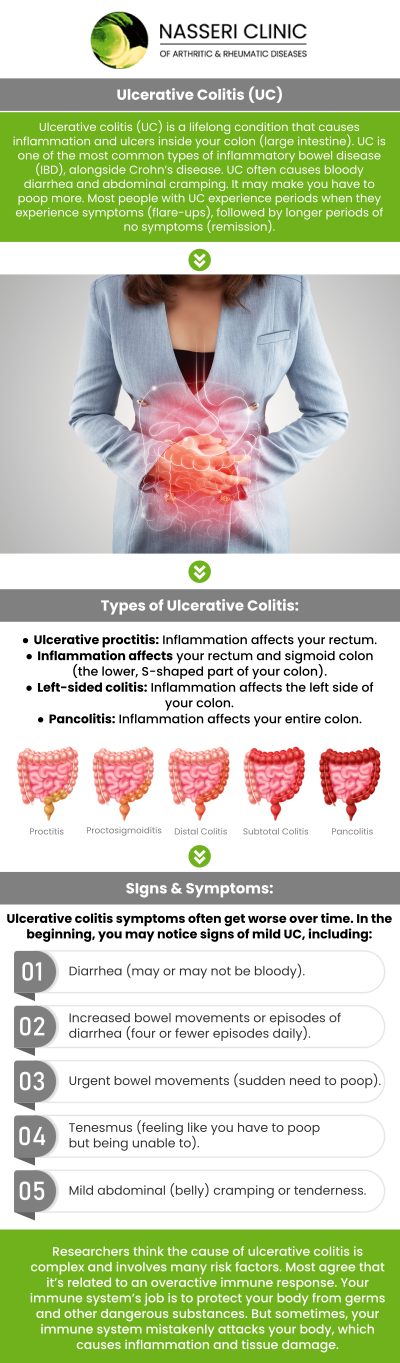
Table of Contents:
What are the common symptoms of ulcerative colitis compared to general digestive issues?
How can I tell if my digestive symptoms are caused by ulcerative colitis or another condition?
How does ulcerative colitis differ from Crohn’s disease and IBS?
When should I see a specialist if I suspect ulcerative colitis?
Could Your Digestive Symptoms Be Ulcerative Colitis? Consult Dr. Nasser Nasseri, MD
General digestive issues—like occasional bloating, gas, or “upset stomach”—usually follow a specific trigger, such as a heavy meal or stress, and typically resolve within a day or two. Ulcerative Colitis (UC), however, is a chronic inflammatory bowel disease (IBD) that causes long-lasting inflammation and ulcers in the innermost lining of your large intestine (colon) and rectum.
The symptoms of UC are often more severe and persistent than general indigestion. They include:
• Urgency and Frequency: A sudden, overwhelming need to have a bowel movement, often resulting in small amounts of stool multiple times a day.
• Rectal Bleeding: Finding blood in the stool or noticing bright red blood on the tissue.
• Abdominal Cramping: Intense, localized pain that often precedes a bowel movement.
• Systemic Symptoms: Unlike a standard stomach bug, UC can cause unexplained weight loss, extreme fatigue, and even low-grade fevers as the body fights the internal inflammation.
Self-diagnosis is notoriously difficult with GI issues because the symptoms overlap with many other ailments. However, there are a few “red flags” that suggest an inflammatory autoimmune cause rather than a simple food intolerance:
• Nocturnal Symptoms: If your digestive pain or the need to use the bathroom wakes you up in the middle of the night, it is rarely “just something you ate.”
• Duration: General issues come and go. UC symptoms tend to persist for weeks or months in a “flare,” followed by periods of remission.
• Extra-intestinal Manifestations: Because UC is an autoimmune condition, it can affect parts of the body outside the gut. Many patients at Nasseri Clinic of Arthritic and Rheumatic Diseases seek help for joint pain, skin rashes, or eye inflammation that occurs alongside their digestive struggles.
It is vital to distinguish between these three conditions because the treatment paths are vastly different.
• Ulcerative Colitis vs. Crohn’s Disease: Both are types of Inflammatory Bowel Disease (IBD). However, UC is limited strictly to the colon and rectum, affecting only the surface lining in a continuous stretch. Crohn’s disease can occur anywhere from the mouth to the anus and can skip sections of the gut, often penetrating deeper into the intestinal walls.
• UC vs. IBS (Irritable Bowel Syndrome): This is the most common confusion. IBS is a functional disorder, meaning the gut looks normal but doesn’t move correctly. It does not cause inflammation, ulcers, or permanent damage to the tissue. UC is an inflammatory disorder where the immune system is actively damaging the physical structure of the colon.
You should schedule a consultation if you experience a persistent change in your bowel habits or if you notice blood in your stool. Early intervention is critical; untreated UC can lead to severe complications, including perforated colon, severe dehydration, and an increased risk of colon cancer.
At our North Baltimore location, we recommend a specialist evaluation if:
• Your symptoms have lasted longer than two weeks.
• You are experiencing “tenesmus” (the feeling that you need to pass stool even though your bowels are empty).
• Standard dietary changes (like going gluten-free or dairy-free) have had zero impact on your pain levels.
• You have a family history of autoimmune diseases or IBD.
At Nasseri Clinic of Arthritic and Rheumatic Diseases, we look at the whole person, not just the symptoms. Dr. Nasser Nasseri, MD, is an expert in managing complex autoimmune and inflammatory conditions that often bridge the gap between rheumatology and gastroenterology. Our approach to Ulcerative Colitis involves precision diagnostics, including specialized lab work and advanced imaging, to map the extent of your inflammation. Dr. Nasseri and his team prioritize finding the most effective biologic or infusion therapies to induce remission and prevent future flares. We are committed to providing a supportive environment in North Baltimore where you can discuss your concerns openly and receive a roadmap back to digestive comfort.
Living with chronic digestive pain is not something you have to do alone. Visit Nasseri Clinic of Arthritic and Rheumatic Diseases for a comprehensive evaluation to determine if your symptoms are related to Ulcerative Colitis or another inflammatory condition. Our team is dedicated to providing you with the answers and the personalized treatment plan you need. For more information, contact us or book an appointment online. We are conveniently located at 3333 N. Calvert St, Suite 540B, Baltimore, MD 21218. We serve patients from North Baltimore MD, Dundalk MD, Halethrope MD, Ferndale MD, Yorktown MD, and surrounding areas.
Check Out Our 5 Star Reviews


Additional Services You May Need

Additional Services You May Need
▸ Arthritis Care
▸ Infusion Therapy
▸ Lab Services
▸ Radiology
▸ NCARD NRACE
▸ BioFlex Laser Therapy
▸ Ultrasound Guided Injection
▸ NCARD PRP
▸ NCARD Myers
▸ Rheumatology
▸ Myositis
▸ Osteoporosis
▸ Ulcerative Colitis
▸ Multiple Sclerosis
▸ Saphnelo Infusion
▸ Injection Treatments
▸ Intravenous Immunoglobulin Therapy
▸ Asthma
▸ Crohn’s Disease
▸ Fibromyalgia
▸ Infusion Therapy for Gout
▸ Inflammatory Eye Disease
▸ Inflammatory Skin Disease
▸ Vasculitis
▸ Iron Deficiency
▸ Lupus
▸ Toradol Injections